Socioeconomic bias in testing and diagnostics of COVID-19
We have a new paper looking at the demographic, epidemiological and clinical characteristics of the first 3 months of COVID-19 in Brazil, a country with one of the fastest-growing COVID-19 epidemics in the world. The study brings some really interesting results that help us (1) understand how Brazil has screwed things up got to this point, and (2) put things in an international perspective.
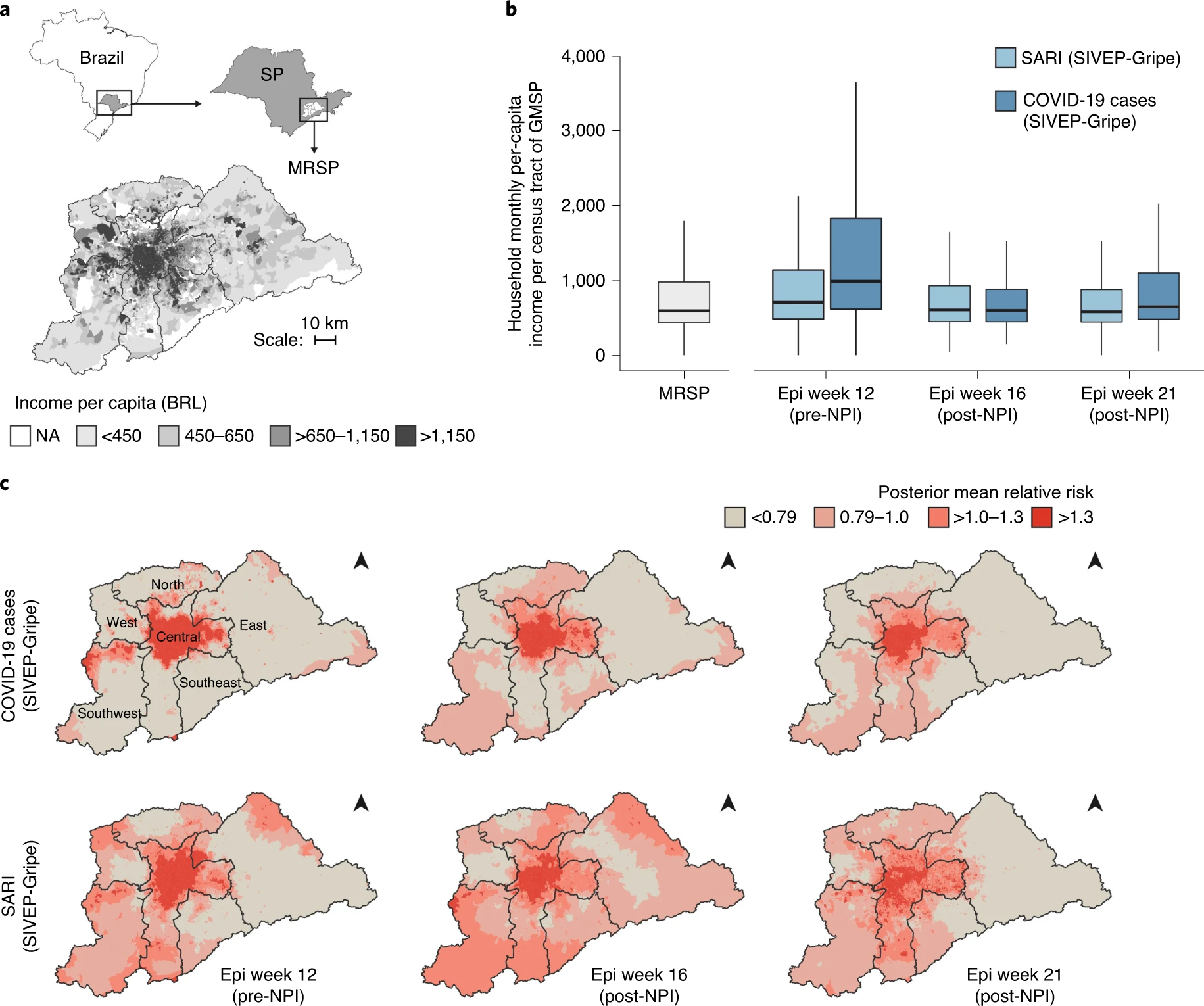
There is one finding I would like to highlight, though. In this study we find an important socioeconomic bias in access to COVID-19 diagnosis. Looking at the metropolitan region of São Paulo, we find that reported cases of severe acute respiratory infection (SARI) are much more likely to be diagnosed with COVID-19 for patients who live in high-income census tracts. Patients living in low-income urban peripheries, on the other hand, are much more likely to be reported with SARI with unknown cause. This can be explained in part by: (1) the high proportion of early cases in returning travelers with higher income and better access to private laboratories for diagnostics; and (2) the more limited access to freely available diagnostic screening. This finding suggests that the true burden of the epidemic in lower-income neighborhoods an vulnerable population groups is probably underestimated.
This study is another great collective effort from a group of researchers from Brazil and the UK under the CADDE project. Thanks William de Souza, Nuno Faria and Ester Sabino for leading the team on this one!
de Souza, W. M., et al (2020). Epidemiological and clinical characteristics of the COVID-19 epidemic in Brazil. Nature Human Behaviour, 1–9. https://doi.org/10.1038/s41562-020-0928-4
Abstract
The first case of COVID-19 was detected in Brazil on 25 February 2020. We report and contextualize epidemiological, demographic and clinical findings for COVID-19 cases during the first 3 months of the epidemic. By 31 May 2020, 514,200 COVID-19 cases, including 29,314 deaths, had been reported in 75.3% (4,196 of 5,570) of municipalities across all five administrative regions of Brazil. The R0 value for Brazil was estimated at 3.1 (95% Bayesian credible interval = 2.4–5.5), with a higher median but overlapping credible intervals compared with some other seriously affected countries. A positive association between higher per-capita income and COVID-19 diagnosis was identified. Furthermore, the severe acute respiratory infection cases with unknown aetiology were associated with lower per-capita income. Co-circulation of six respiratory viruses was detected but at very low levels. These findings provide a comprehensive description of the ongoing COVID-19 epidemic in Brazil and may help to guide subsequent measures to control virus transmission.